What is Skin Tag Removal: Overview, Benefits, and Expected Results
The new product is a great addition to our lineup.
Our latest product is an exciting addition to our already impressive lineup! With its innovative features and sleek design, it's sure to be a hit with customers. Don't miss out on this amazing opportunity to upgrade your life!
What is Skin Tag Removal: Overview, Benefits and Expected Results
Skin tags are small pieces of flesh-colored or darker growths that hang off the skin and they can look like warts, moles or fatty bumps. They are very common and can appear along the neck, armpits, and eyelids. Skin tags usually don’t cause any discomfort and often don’t need any treatment. For those who decide to get them removed for cosmetic reasons, there are several skin tag removal methods such as home-remedies, excision, freezing and laser treatment.
What Causes Skin Tags?
Skin tags develop when the skin rubs together in areas of friction such as where a bra rubs against the skin, in the neck, underarms or groin. Skin tags are also more common in elderly people, pregnant women and those who are overweight.
What Does Skin Tag Remova Look Like?
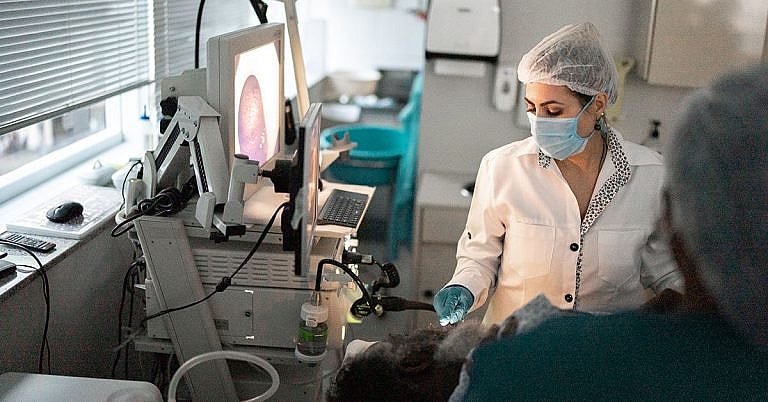
Skin tag removal typically involves an outpatient procedure during which the doctor will cut off the skin tag using a scalpel, scissors or other sharp instrument. Certain laser, cryosurgery or electrocautery may also be used to remove the skin tag. The area may then be treated with a local anesthetic such as lidocaine or injected with anesthetic before the procedure.
Benefits of Skin Tag Removal
The main benefit of having skin tags removed is improved cosmetic appearance. Skin tags are often unsightly and for some can even be distressing. Removing them can restore self-confidence. Other potential benefits of skin tag removal include:
- Eliminates skin tag-related itching or discomfort
- Prevents skin tags from becoming bigger or infected
- Reduces the risk of a skin tag becoming cancerous
How to Prepare for Skin Tag Removal
Before undergoing skin tag removal, it’s important to be seen and assessed by a dermatologist and make sure the skin tag is indeed a harmless skin tag. Skin tags may resemble other, more serious skin conditions such as moles or even skin cancer. The doctor will examine the skin tag to make an accurate diagnosis. Once the diagnosis is confirmed, the doctor can help you decide which removal method is the safest and most effective.
Expected Results of Skin Tag Removal
The results of skin tag removal will vary depending on the size and location of the skin tag. Generally, the skin tag will be removed completely and it won’t return. It’s important to note that the removed skin tag will not be replaced by a new one. However, it’s worth noting that people with a high risk of developing skin tags may continue developing new ones in other areas.
Aftercare
After skin tag removal, the area should be kept clean and dry. To reduce pain and prevent infection, the doctor may suggest applying an antibiotic ointment or keeping the area covered with a special dressing. The skin should heal within a few days, and the doctor should monitor the area to ensure no infection develops.
Risks and Complications
When it comes to skin tag removal, there are a few risks and complications that should be taken into account. The possible risks include:
- Burning of the surrounding skin
- Infection at the site of the skin tag
- Pain and discomfort
- Scarring
Surgical vs Non-Surgical Skin Tag Removal
Surgical Skin Tag Removal
The most common surgical skin tag removal method is excision. This procedure involves using a scalpel, scissors, or other sharp instrument to cut off the skin tag. Other prognoses may involve laser therapy, electrocautery, and cryosurgery.
Non-surgical Skin Tag Removal
Non-surgical skin tag removal typically involves topical medications or home remedies. This is usually reserved for smaller skin tags or for those located in areas where surgery is not recommended. Examples of these medications include:
- Topical gels and creams
- Cryotherapy with liquid nitrogen
- Talcum powder
- Apple cider vinegar
- Tea tree oil
- Ligation with thread or dental floss
The Bottom Line
Skin tag removal is safe and effective and the results are usually permanent. When considering skin tag removal, it’s important to speak to a qualified dermatologist or your doctor to determine the best method for you.
Definition and Overview
A skin tag, medically known as an acrochordon or a fibroepithelial polyp, is a benign tumour, usually small and composed of a fibrotic core covered by skin. These masses typically develop in areas where the skin folds and creases are found, such as the armpit and the neck. Skin tags are usually raised off from the skin, attached via a fleshy stalk known as a peduncle. They are painless masses, and they generally do not grow to significant sizes (typically less than 1 cm).
Skin tags are found in approximately 45% of individuals and are more commonly seen in females than in males. The risk of developing them increases as one gets older. They are believed to develop from the rubbing of skin on skin. Some studies have shown certain kinds of human papillomavirus (HPV), specifically HPV 6 and HPV 11, can be found in skin tags, and may have a role in its formation. Meanwhile, other studies have shown an association of these lesions with insulin resistance and obesity. Thus, some sources have suggested that skin tags may indicate a higher risk for cardiovascular diseases and atherosclerosis. Genetics is also believed to contribute to their development.
Who Should Undergo and Expected Results
A skin tag is a benign lesion. No treatment is necessary unless it:
Becomes irritated or infected, which is usually caused by repeated contact with clothes or jewellery
Interferes with normal functioning. For instance, skin tags on the eyelids may produce eye pain and vision disturbances.
Causes sufficient discomfort to the patient, such as in the case of large skin tags on the thighs that may make it difficult for the patient to walk.
Is linked to squamous cell carcinoma or a basal cell carcinoma – There have been reports of skin tags examined histologically revealing a squamous cell carcinoma or a basal cell carcinoma; however, these are rare instances.
The most frequent indication for skin tag removal is for cosmetic purposes. A skin tag may be removed if the patient prefers to have the procedure done.
How is the Procedure Performed?
Skin tag removal is an office procedure that is usually performed by a dermatologist. For skin tags found in sensitive locations, a specialist may have to perform the removal. For example, a skin tag found on the eyelid may be better removed by an ophthalmologist while a skin tag located in the perianal area is best excised by a surgeon.
There are several techniques for removing a skin tag. These include cauterisation, cryosurgery, ligation, and excision.
Electrocauterisation, which is a treatment option for small skin tags, makes use of high-frequency current that produces heat energy in order to burn the cells of the lesion. Topical anaesthetic is applied to the skin tag, and after several minutes, a heated device known as a cautery probe or pen is made to touch the lesion. The skin tag is burned off and the burnt material is removed. An antibiotic ointment is usually applied to the cauterised area, and patients are advised not to wash the area overnight.
At the other end of the spectrum is cryosurgery, which utilises a special substance, usually liquid nitrogen, to freeze the skin tag. During the procedure, the basement membrane is disrupted, resulting in tissue destruction. The application of the substance on the skin tag may be done using a cotton applicator or a cryoprobe. Some physicians use forceps to grasp the skin tag and apply cryotherapy to the forceps to minimise damage to surrounding normal tissues. The skin tag eventually falls off on its own. This procedure is also ideal for small skin tags.
Both cauterisation and cryosurgery are ablative procedures, which means that tissue is destroyed and cannot be sent for examination.
Other options for the removal of small skin tags include simply cutting the skin tag off using curved scissors, and ligation of the stalk using suture material or a copper wire to cut off the blood supply to the lesion.
Large skin tags, on the other hand, may require excision for complete removal. This requires a minor surgical procedure performed under local anaesthesia. If the stalk is narrow, it can be shaved off with a scalpel and cauterised for hemostasis. The skin reepithelialises after a few days. On the other hand, if the stalk is wide, a fish mouth incision may be done around the stalk, up to the dermis. A small amount of normal skin may be removed together with the skin tag. The remaining skin is then sutured together.
Possible Risks and Complications
There are very few risks associated with skin tag removal, and complications are minor. Bleeding and infection rarely occur while pain and soreness are minimal, especially if the skin tags are small. Pain can usually be managed with over-the-counter pain medications. Redness and swelling can likewise occur but typically resolves on their own.
The usual complication of skin tag removal is related to scar formation. Cryotherapy of skin tags may result in discoloration of the skin but is usually temporary. Small scars may also be left after skin tag removal. For most people, wound healing is unremarkable, and the scar is barely visible. However, if the patient is prone to developing hypertrophic scars or keloids, the scar may become dystrophic, resulting in poor cosmetic outcomes. Unpleasant scars may be managed via several ways, including the application of special creams, steroid injections, and surgical revision.
Fibroepithelial polyps are not known to recur; however, some patients who are prone to developing skin tags can develop new lesions, which may require repeat treatments.
References:
Savage JA, Maize JC Sr. Keratoacanthoma clinical behavior: a systematic review. Am J Dermatopathol. 2014 May. 36(5):422-9
Papp DF, Khanna AJ, McCarthy EF, Carrino JA, Farber AJ, Frassica FJ. Magnetic resonance imaging of soft-tissue tumors: determinate and indeterminate lesions. J Bone Joint Surg Am. 2007 Oct. 89 Suppl 3:103-15.
/trp_language]
[trp_language language=”ar”][wp_show_posts id=””][/trp_language]
[trp_language language=”fr_FR”][wp_show_posts id=””][/trp_language]







Great info!
Super helpful – thank you!
Great info! Super helpful – thank you! #usefulinformation